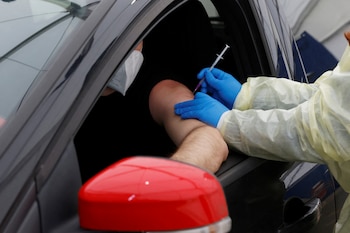
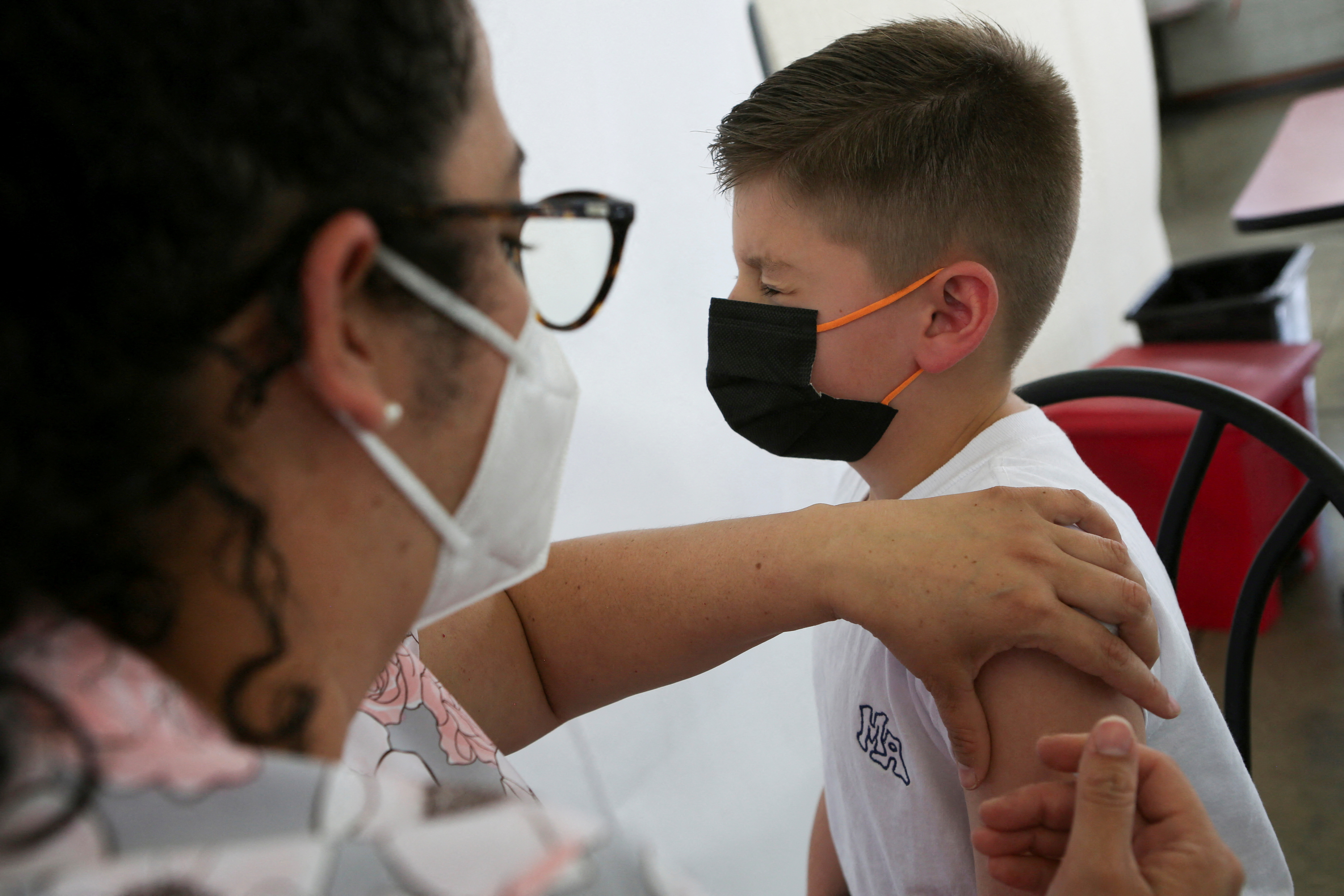
People who had been infected with the coronavirus and accessed doses of COVID-19 vaccines have “hybrid immunity”. There are already 4 scientific studies that provide evidence that these vaccines provide important additional protection to these people.
Vaccines have already been shown to be very effective in protecting people who have never had COVID-19, but their effectiveness in preventing symptoms and severe outcomes in people who have already had been infected was, until recently, less clear.
PUBLICIDAD
After two years of a pandemic in which nearly 500 million people have been infected and 59% of humanity have been vaccinated with the primary scheme - according to information from OurWorldIndata -, studies have highlighted the importance of being vaccinated for those who have natural immunity after recovering from the disease.
One of the two studies published in the medical journal The Lancet Infectious Diseases analyzed the health data of more than 200,000 people, between 2020 and 2021, when Brazil was most affected by the coronavirus , being the second country in the world with the highest number of deaths from COVID.
PUBLICIDAD
Researchers from Brazil found that in people who have already had COVID-19, the Pfizer and AstraZeneca vaccines were 90 percent effective against hospitalization and death, China's CoronaVac vaccine was 81 percent, and Johnson & Johnson's single-dose inoculant was 58 percent.
“All four vaccines have been shown to provide significant additional protection to those with previous COVID-19 infection,” said study author Julio Croda, of the Federal University of Mato Grosso do Sul.
PUBLICIDAD

“Hybrid immunity due to exposure to natural infection and vaccination is likely to be the norm worldwide and could provide long-term protection even against emerging variants,” said Pramod Kumar Garg, of the Indian Institute of Translational Health Science and Technology, in a related commentary to the studio.
PUBLICIDAD
Meanwhile, another study that used Sweden's national registry until October 2021 found that people who recovered from COVID retained a high level of protection against re-infection up to 20 months. And it also found that people with hybrid immunity from two doses of vaccines had a 66% lower risk of re-infection than those with only natural immunity.
Paul Hunter, professor of medicine at the University of East Anglia who did not participate in the study, told AFP that the 20 months of “very good protection” of natural immunity was “much better than would be expected for the original two-dose vaccine schedule.” But he warned that both studies were conducted before the Ómicron variant became dominant worldwide, and that it had “markedly decreased the protective value of a previous infection.”
PUBLICIDAD

A study conducted in Qatar and published on the MedRXIV pre-publication website last week revealed the protection offered by hybrid immunity against Ómicron. He found that three doses of the vaccine were 52% effective against symptomatic infection of the BA.2 Omicron subvariant, but that figure skyrocketed to 77% when the patient had been previously infected.
PUBLICIDAD
The study, which has not been peer-reviewed, concluded that “hybrid immunity resulting from previous infection and recent booster vaccination confers the greatest protection” against subvariants BA.1 and BA.2.
Also in the United States, Marion Pepper, associate professor in the Department of Immunology at the University of Washington School of Medicine, published other research in the journal Cell and explained why “hybrid immunity” gives better protection. They compared differences in the immune response to coronavirus across three doses of the vaccine in 30 people who had been previously infected and in 24 who had been vaccinated but never infected.
PUBLICIDAD
They found that, after vaccination, those who had been previously infected generated more memory B cells, which generate antibodies that can neutralize the virus and prevent infection. These memory B cells in people with hybrid immunity also generated a greater variety of antibodies that can not only neutralize the original strain of the virus, but also newer variants such as Delta and Omicron.
“Even if their first infection was caused by the oldest strain, the Wuhan strain, and the vaccine they received was based on that strain, people with hybrid immunity were able to generate neutralizing antibodies against each variant,” Pepper said.
PUBLICIDAD
Hybrid immunity also generated a more specific cellular immune response to combat viral infections, called the Th1 response. In this response, immune cells called CD4+ T cells release inflammatory signals, namely a cytokine called interferon-gamma that is antiviral. CD4+ T cells from previously infected individuals were also found to produce more Interleukin-10, which can suppress inflammation and potentially prevent pathology.
“While additional vaccination was able to increase the number of CD4+ T cells in which they had not been infected to levels that had been infected, it could not generate the same quality of CD4+ T cell response seen in those with hybrid immunity,” Pepper said.

Several factors could explain why hybrid immunity seems more robust. One factor could simply be time. Upon exposure to a pathogen, immune cells in the lymph nodes refine the immune response. This process of immune maturation generates more effective antibodies and cells against the new infection.
In the case of the hybrid immunity group, a year passed from the moment of infection until they received the vaccine. In contrast, individuals in the vaccine-only group received their second dose only a few weeks after the first dose, which gave the immune system much less time to refine its response.
Another factor may be where the immune system first interacts with an invading pathogen. Different parts of the body have different environments that determine how the immune system responds to infection. The immune cells of the study participants with hybrid immunity were first found with the virus in their lungs and nasal passages. In contrast, cells from the vaccine-only group were first found with the viral protein in the muscle where they received the vaccine.
Exposure to the lungs and mucosal tissues, such as those found in the nasal passages, is likely to generate a better immune response to a respiratory pathogen because cells may be better retained in these locations, Pepper said. His group's findings could help scientists design vaccines that take advantage of this effect, such as those that can be administered into the nasal passages or inhaled directly into the lung.
Although vaccination after a previous infection appears to produce a greater immune response to SARS-CoV-2 infection, it is essential that people who have been infected get vaccinated to get this benefit, Dr. Pepper advised. “People who have had COVID-19 should definitely get vaccinated. Not only does immunity to infection decrease over time, but vaccination is also necessary to create this hybrid immunity,” he added. His research was supported by the National Institutes of Health, the Burroughs Wellcome Fund and Emergent Ventures.
While “hybrid immunity” provides better protection, the chief scientist of the World Health Organization (WHO), Dr. Soumya Swamin, warned that caution should be maintained. “Hybrid immunity doesn't mean people should let their guard down with the mask, distancing and hand hygiene,” he said. His recommendation is because it is not known how long the natural immunity from infection can last in each person and in addition vaccines do not prevent 100% of infections. “In addition, a person can have the coronavirus even if they are vaccinated,” he said.
KEEP READING:
PUBLICIDAD
PUBLICIDAD
Últimas Noticias
Debanhi Escobar: they secured the motel where she was found lifeless in a cistern
Members of the Specialized Prosecutor's Office in Nuevo León secured the Nueva Castilla Motel as part of the investigations into the case

The oldest person in the world died at the age of 119
Kane Tanaka lived in Japan. She was born six months earlier than George Orwell, the same year that the Wright brothers first flew, and Marie Curie became the first woman to win a Nobel Prize

Macabre find in CDMX: they left a body bagged and tied in a taxi
The body was left in the back seats of the car. It was covered with black bags and tied with industrial tape
The eagles of America will face Manchester City in a duel of legends. Here are the details
The top Mexican football champion will play a match with Pep Guardiola's squad in the Lone Star Cup

Why is it good to bring dogs out to know the world when they are puppies
A so-called protection against the spread of diseases threatens the integral development of dogs



